The assessment of the patient's airway is an integral part of the pre-operative workup. Its purpose is to predict potential problems, allowing a management plan to be developed ahead of time and avoid an unanticipated difficult airway.
Basically, the aim is to predict and therefore plan ahead for potential problems in two areas:
- Laryngoscopy and intubation, and more importantly ...
-
Ventilation, i.e. oxygenation, which means ease of ...
- Bag-mask ventilation
- Oxygenation with a supraglottic airway as a rescue technique
- Oxygenation with a infraglottic airway/ FONA as a last resort
Predicting difficulties with ventilation and oxygenation is more important than predicting difficulties with laryngoscopy. Failed laryngoscopy or intubation is not inherently dangerous if you can oxygenate your patient.
In addition to identifying relevant patient factors, preoperative airway assessment should also take into account the type of surgery planned and its impact on the type of anesthesia required. This is particularly important in operations with a 'shared airway'. Communicate with your surgeon!
Airway management problems continue to be the single most common cause of morbidity and mortality attributable to anesthesia! In addition, these are problems that you own exclusively as an anesthesia provider. There is very little blame sharing in avoidable airway management mishaps.
The Australian and New Zealand College of Anaesthetists (ANZCA) has put together an excellent document on preoperative airway assessment.
ANZCA suggests a list of 9 essential questions or "core considerations" which need to be adressed during preoperative airway assessment:
- Is there information about any previous airway difficulties?
- Is there any altered cardiorespiratory physiology?
- What is the impact of the surgery on the airway?
- How difficult will it be to bag-and mask ventilate?
- How difficult is it to place a supraglottic airway?
- How difficult will it be to intubate the patient?
- How difficult will it be to perform an infraglottic airway?
- What is the risk of aspiration?
- How easy will they be to extubate safely?
Like any kind of patient evaluation preoprative airway assessment can be divided into history and examination, supported by clinical tests.
The Australian VORTEX appraoch website has a fantastic page on preoperative airway assessment and planning. Do yourself a favor and check it out!
HISTORY
Previous airway management problems
"The best predictor of future behavior is past behavior."
Look at old anesthetic records, if they are available, to see if problems with airway management were documented. In practice this means finding comments on ease or difficulty of bag-mask ventilation, laryngoscopy view, and any special airway techniques or equipment used previously. You might even consider requesting records from a different hospital if airway management is expected to be particularly challenging and time allows.
Ask the patient! Although it is unlikely that a patient will be able to provide details about why airway management was difficult in the past, statements such as ' they we're struggling to get the tube down' or similar should obviously ring alarm bells.
Previous interventions/ surgeries/ therapies potentially affecting airway management
Find out if the patient has had head/ neck surgery before such as laryngeal surgery, neck dissection, facial reconstruction, tracheotomy or c-spine surgery. A particular large red flag is the history of radiotherapy to the neck!
Consider whether a patient had any of these interventions or treatments since the last documented 'uneventful intubation'.
Aspiration risk
Certain patients are at an increased risk of regurgitation and aspiration of stomach contents such as food particles or gastric acid because of conditions such as GERD, hiatal hernia, obesity, autonomic neuropathy, non-npo status, etc. While these conditions do not affect the mechanical aspects of airway management per se, an increased aspiration risk might lead you to consider specific airway management techniques, e.g. a rapid sequence induction, which in themselves have certain (higher) risks.
Obstructive sleep apnea (OSA)
OSA has been identified as an independent risk factor for difficult bag-mask ventialtion and intubation. Ask your patient if they had a formal diagnosis of OSA, which requires a sleep study, and if they use home CPAP.
You are likely to come across patients who have not definitiely been diagnosed with OSA but in whom you strongly suspect it. A screening score such as the STOP-BANG assessment, developed by the University Health Network in Toronto, CA, is helpful in identifying likely OSA cases and guide overall risk stratification.
These are the questions for the STOP-BANG score:
- Do you Snore loudly (loud enough to be heard through closed doors or your bed-partner elbows you for snoring at night)?
- Do you often feel Tired, Fatigued, or Sleepy during the daytime (such as falling asleep during driving or talking to someone)?
- Has anyone Observed you Stop Breathing or Choking/Gasping during your sleep?
- Do you have or are being treated for High Blood Pressure?
- Body Mass Index more than 35 kg/m2?
- Age older than 50?
- Neck size large? (Measured around Adam's apple)
- Gender = Male?
Low Risk: Yes to 0 - 2 questions
Intermediate Risk: Yes to 3 - 4 questions
High Risk: Yes to 5 - 8 questions or Yes to 2 or more of 4 STOP questions + male gender
or Yes to 2 or more of 4 STOP questions + BMI > 35kg/m2
or Yes to 2 or more of 4 STOP questions + neck circumference 17 inches/ 43cm in male or 16 inches/ 41cm in female
Obesity
Obesity has several adverse effects on bag-mask ventilation and laryngoscopy, which are discussed in the page 'Special patient circumstances' - 'The obese patient'.
Altered cardio-respiratory physiology
Like an increased aspiration risk, cardio-respiratory disease does not affect the mechanical aspects of airway management per se. It might affect you ariway management plan though as you have to anticipate a range of issues such as reduced tolerance of apneic time during intubation or reduced tolerance of tachycardia/ hypertension as a sympathetic response to laryngoscoopy/ intubation.
EXAMINATION & CLINICAL TESTS
Like any diagnostic tool, an ideal method of preoperative airway assessment should have high sensitivity and specificity, while maintaining a high predicitve value. Disappointingly, no single test for airway assessment meets these requirements!
Click here for an excellent editorial on predicting the risk of difficult intubation, and the problems all tests suffer with regards to sensitivity, specificity, and predictive value.
More on predicting risk below ...
This is not an exhaustive list of tests. Others not mentioned here have been described and used.
Dental status
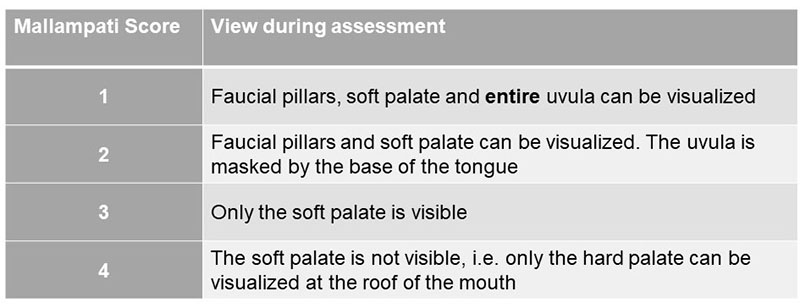
Mallampati score
Mouth opening/ inter-incisor gap (IIG)
Thyromental distance (TMD)
Temporomandibular joint (TMJ) mobility
Neck mobility
Transnasal flexible endoscopic laryngoscopy (TFEL)
Other patient features
A possible sequence for the preoperative airway exam
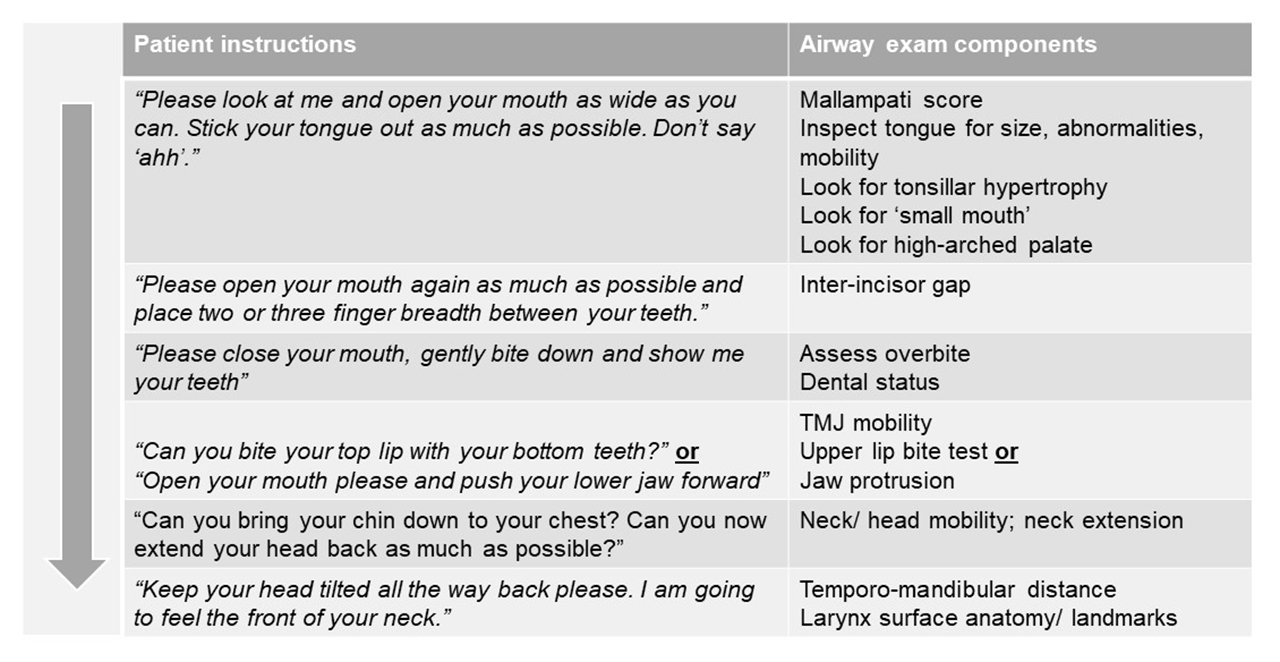
It is probably fair to say that no two anesthesia providers will do their preoperative airway exam exactly the same way. One suggested sequence is outlined in the table below:
PREDICTING DIFFICULT INTUBATION AND VENTILATION- THE VALUE OF TESTING
Assessing the airway before surgery using some combination of the tests described above is standard clinical practice. But how good are these tests on their own or in combination to predict which patients will be truly difficult to ventilate and/ or intubate and which ones won't? Unfortunately there is no way to talk about tests and the value of testing without some basic statistical knowledge. Familiarize yourself again with the concepts of sensitivity, specificity, positive predictive value and negative predictive value!
What are the sensitivities, specificities and positive predictive values of the commonly used tests described above?
- Mallampati score: This is arguably the most recognized and most performed test for preoperative airway assessment. Depending on which validation study you read, sensitivity is between 40- 80%, specificity is between 50 - 85%, and the positive predictive value (PPV) is between 5- 20%.
- Inter-incisor gap (IIG): Mouth opening has a sensitivity of around 25- 45%, a specificity of around 95%, and a PPV of up to 25%.
- Thyromental distance (TMD): Depending on the study, sensitivity is quoted to be between around 5% and 90%, specificity ranges from roughly 25% to 80%, and PPVs from about 15% to 40% have been found.
- TMJ mobility: Sensitivity is up to 30% at best, specificity is 85% to 90%. Like for the other tests, the PPV is low being around 20%.
- Neck mobility:
It is immediately obvious that many tests have relatively low sensitivity although they are largely fairly specific. Even more concerning though is the fact that their positive predictive value is generally very low. This is because truly difficult intubations are comparatively rare. The PPV of a test always suffers when the condition it aims to predict is rare!

Combinations of tests perform somewhat better. For example, the Mallampati score together with the thyromental distance achieved around 80% sensitivity, 98% specificity and a PPV of almost 65% in one study (the PPV was so much higher because of the high specificity of this test combo).
Scoring systems
One example of a scoring systems for preoperative airway assessment is the Wilson risk sum score. Others include the Arne risk index or the El-Ganzouri risk index. Neither are widely used in clinical practice but apply more in research settings to describe patient or study populations:
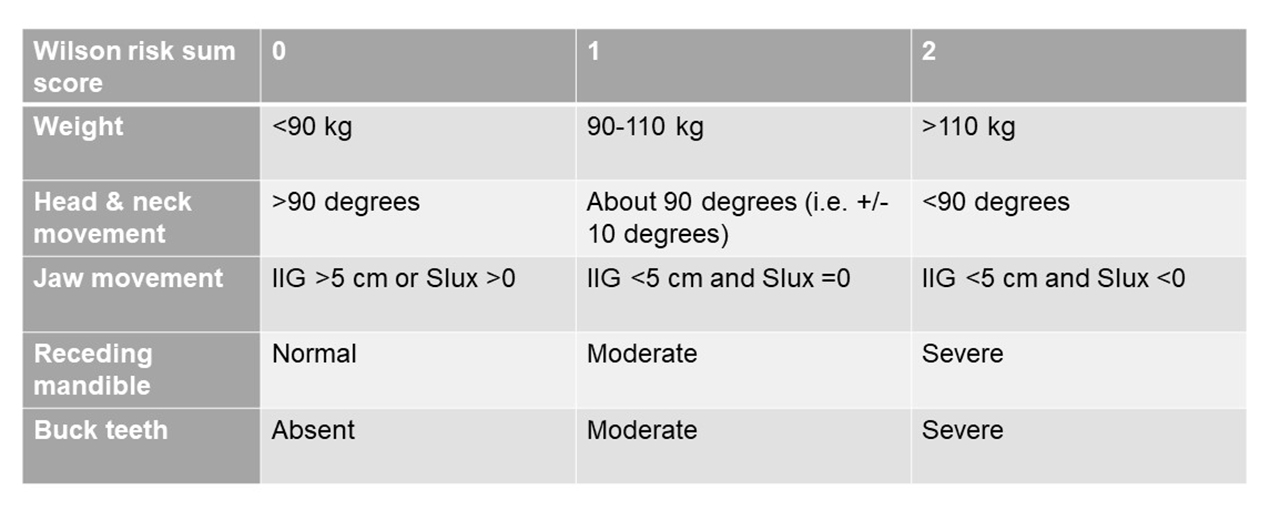
Even with this combination of tests, while the sensitivity and specificity of the Wilson risk score are up to 55% and 90% respectively, the PPV is still only about 10%.
The 'value' of the preoperative airway assessment
Given that the positive predictive value of preop airway assessment test if overall low, even when used in combination, is there much point in doing any kind of assessment at all? Is it a waste of time? To quote from Yentis (2002): "To this I say no, for there is another important benefit of this ritual: It forces the anaesthetist at least to think about the airway, and for this reason we should encourage our trainees (and ourselves) to continue doing it. What we must do is dispel the myth that it actually helps us in predicting dificulty accurately, and have a clear idea about what we are going to do if a test suggests a patient may be difficult, knowing that they probably won't be."
SITUATIONAL AWARENESS
There are some easily overlooked aspects of preoperative airway assessment because they go beyond the more familiar medical history and examination discussed above and have more to do with logistics. They are nevertheless crucial to the development of your airway management plan, just as the assessments described above are.
- Where are you going to do your airway interventions? Operating room, ED, ward, ICU, out-of-hospital setting, ...? Are you familiar with the location?
- What equipment is available? What needs to be brought from some place else? How long will that take? Can the patient be adequately positioned for airway management (be particularly weary of CT scan, angiography tables that do not allow head elevation or reverse Trendelenburg positioning)?
- Who else is on your team? Do you know what their skillset is? What is yours, might you need help? Would help be available?
REFERENCES
Mallampati, S. R.; Gatt, S. P.; Gugino, L. D.; Desai, S. P.; Waraksa, B.; Freiberger, D.; Liu, P. L. (1985): A clinical sign to predict difficult tracheal intubation: a prospective study. In Canadian Anaesthetists' Society Journal 32 (4), pp. 429–434. DOI: 10.1007/BF03011357.
Gemma, Marco; Buratti, Luca; Di Santo, Davide; Calvi, Maria R.; Ravizza, Alfredo; Bondi, Stefano et al. (2020): Pre-operative transnasal endoscopy as a predictor of difficult airway: A prospective cohort study. In European Journal of Anaesthesiology 37 (2), pp. 98–104. DOI: 10.1097/EJA.0000000000001127.




Comments
Dear Claas, this is great. I
Dear Claas, this is great. I was looking for a resource to teach my medical student the airway exam and this is perfect.
Add new comment